Professionals within the clinical genomics system recognise the significant benefits of genomics in healthcare, but they hold divergent perspectives on the ethical, technical, and social risks involved.
Australia is making rapid progress integrating genomics technologies into clinical practice with the overarching aim of delivering better healthcare treatment options and patient outcomes. However, the use of any new suite of technologies requires a governance approach that supports robust assessment, categorisation, communication, and management of any associated risks.
Clinical genomics is also a system comprised of multiple stakeholders and institutions. Yet there is little research that examines the comparative perspectives of those working in and shaping the field.
In a recent study published in New Genetics and Society, researchers from CSIRO’s Responsible Innovation Future Science Platform and Transformational Bioinformatics Program engaged four groups of professionals - clinical geneticists, genetic counsellors, laboratory professionals (pathologists and bioinformaticians), and researchers - to find out how they understood and expressed the benefits and the risks of clinical genomics in Australian healthcare.
The research found that professionals hold strong agreement on the benefits of integrating clinical genomics into healthcare. These benefits were largely associated with improving the diagnosis and prediction of diseases and developing more targeted treatments. However, they hold more diverse perspectives on the potential risks associated with clinical genomics.
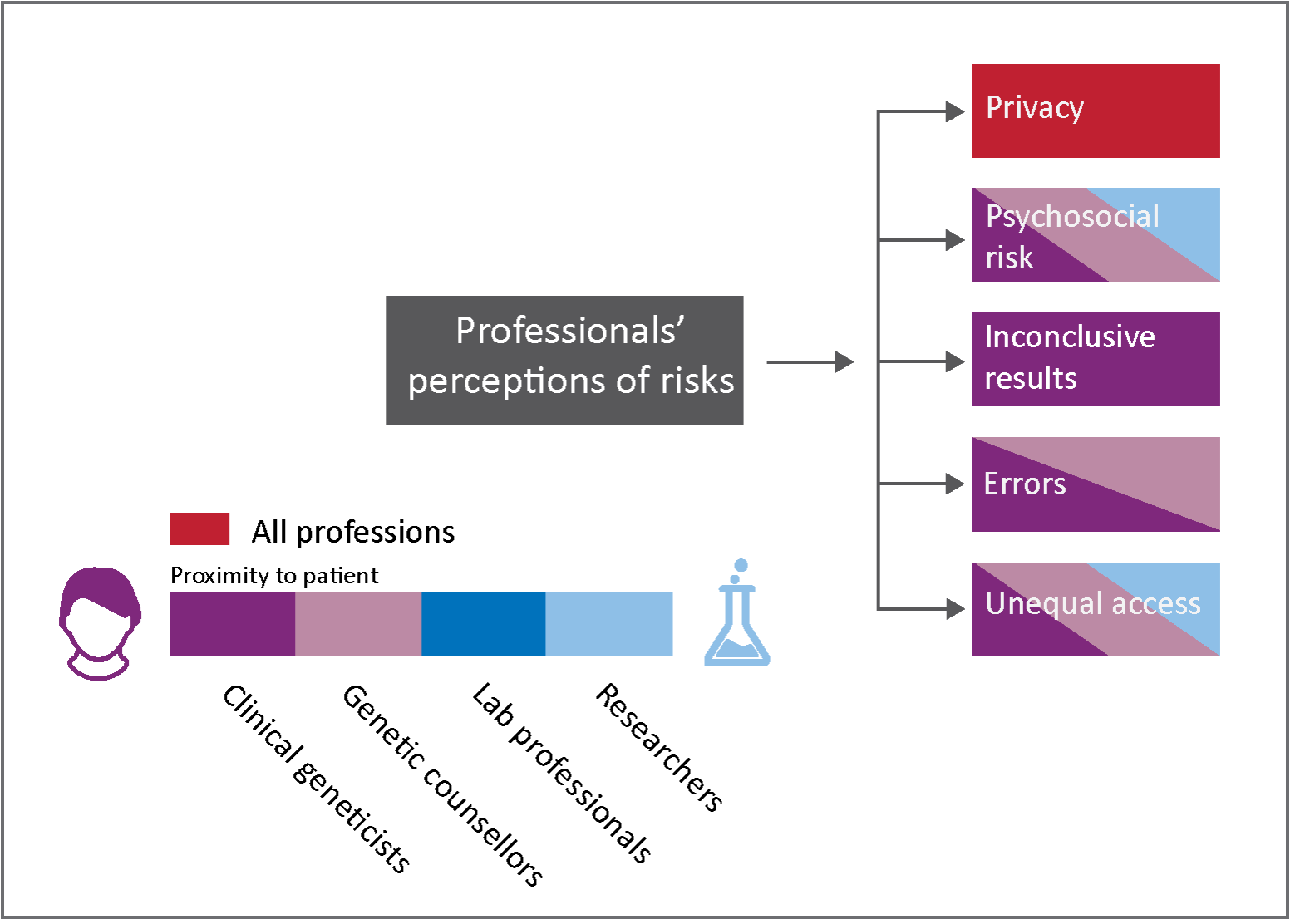
Multidimensional view of risks
"The value in identifying a diverse range of perceived risks among professionals working across a broader system is that it can mitigate the potential for miscommunication or misinterpretation of the value proposition of clinical genomics,” explains lead author, Dr Yuwan Malakar.
The study identified a range of perceived risks associated with clinical genomics that are distributed across ethical (such as privacy and psychosocial risks), technical (inconclusive results and errors), and social (unequal access) risk domains.
Risks to privacy were identified almost unanimously across the professional categories, and included issues such as data leakage, identifiability, misuse, discrimination, and the potential for unintended data reuse. This confirmed some key issues that have been reported in the literature.
However, the identification of technical risks was more nuanced across the professions. In terms of inconclusive results, participants recognised that limitations in both technology and reference databases were contributing factors, but clinical geneticists perceived the impact of the risk differently to researchers, for example.
Dr Malakar said, "These wider perceptions provide a foundation for identifying a broader range of risks among stakeholders. This broader understanding is crucial for developing more comprehensive and responsible approaches to risk mitigation in the delivery of clinical genomics."
Towards risk governance of clinical genomics
The research also suggests that perceptions of risk are influenced by participants' professional roles. There were clear differences observed between the type of risks perceived between those working directly with patients (clinical geneticists and genetic counsellors) and those working “behind the scenes” (laboratory professionals and researchers).
"Quantifying the differences in opinion along the value chain of clinical genomics helps identify gaps in knowledge and conflicting priorities, which in turn can improve connection points", said A/Prof Bauer.
Identifying these diverse perceptions of risk can help professionals in their respective roles and aid collaborative efforts to manage risk and responsibility effectively.
References
Subscribe to Transformational Bioinformatics
Stay up-to-date with our progress


